Peroneal Tendon Rehab Protocol
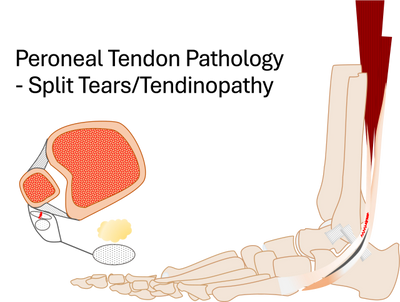
Peroneal Tendon Repair Rehabilitation Protocol (Standard Track)
Applies to: peroneal tendon debridement/repair, tubularization, tenosynovectomy, SPR work (if performed, be more conservative with eversion/subluxation risk), without major tendon transfer/graft/osteotomy.
Phase 0: Protection and Recovery (0 to 2 weeks)
Immobilization / WB
- Posterior splint (or short leg splint) with ankle in neutral to slight plantarflexion per surgeon preference.
- Non-weight-bearing (NWB) with crutches/knee scooter.
Goals
- Protect the repair, reduce swelling, control pain.
- Maintain conditioning (core/hip/knee), maintain toe motion.
Therapeutic exercise
- Toe AROM, gentle intrinsic foot activation (within dressing limits).
- Knee ROM, hip strengthening, contralateral limb conditioning.
- No active ankle eversion.
Precautions
- Keep incision dry, elevate aggressively.
- Avoid inversion/eversion stresses and resisted peroneal activation.
Evidence note: A commonly reported pattern is splinting briefly followed by ~2 weeks NWB casting/splinting, then transition to boot/cast with progressive WB depending on surgeon preference.
Phase 1: Early Motion in Boot (2 to 6 weeks)
At ~2 weeks
- Wound check, suture removal.
- Transition to CAM boot.
Weight-bearing
- Begin progressive weight-bearing in boot as tolerated (typical: partial → full by 4–6 weeks if swelling/pain allow and fixation/repair quality supports it).
ROM
- Start gentle ankle AROM/PROM for:
- Dorsiflexion / plantarflexion
- Inversion (gentle), and avoid combined inversion + plantarflexion stress
- NO aggressive active eversion (your preference: avoid until 6 weeks)
- Begin active inversion / dorsiflexion / plantarflexion at 2 weeks (as you outlined), emphasizing smooth, low-load motion.
Strength
- Proximal strengthening (hip/core), closed-chain work only as allowed by WB status.
- No resisted eversion and no peroneal strengthening yet.
Manual therapy
- Scar mobilization once incision healed.
- Gentle joint mobilizations as needed (avoid stressing lateral ankle/peroneals).
Criteria to progress
- Minimal swelling, pain controlled.
- Tolerating progressive WB in boot.
- DF/PF ROM improving without lateral tendon pain.
Phase 2: Strength Initiation and Gait Normalization (6 to 12 weeks)
Weight-bearing / bracing
- Wean boot to supportive shoe when:
- You can walk pain-minimized in boot with normalized gait and minimal swelling.
- Consider a lace-up ankle brace for transition and higher-demand walking.
ROM
- Progress to full ROM in all planes as tolerated.
- Start gentle stretching (gastroc/soleus) but keep it symptom-guided.
Strength (start peroneals now)
- Begin active eversion (unresisted → light band) starting at ~6 weeks.
- Progress to:
- Eversion isometrics → isotonic bands
- Heel raises (double → single)
- Balance/proprioception (single-leg stance, foam, perturbations)
Functional
- Stationary bike / elliptical as tolerated.
- Pool running once wounds healed and gait mechanics are safe.
Evidence note: Many published pathways initiate formal PT and strengthening around ~6 weeks once protective immobilization ends, then restore ROM/strength progressively. (PMC)
Phase 3: Return to Running and Sport (3 to 6 months)
Advanced strengthening
- Single-leg heel raises endurance, lateral step-downs, controlled hopping progressions.
- Eccentric calf strengthening and peroneal endurance.
Running progression (typical)
- Begin treadmill walk-jog progression when:
- Pain minimal, no reactive swelling
- Near-symmetric ROM
- Good single-leg balance/control
- Advance to cutting/pivoting and sport-specific drills later.
Return-to-sport criteria (practical)
- Pain-free functional hopping progressions.
- Symmetric single-leg heel raises and balance testing.
- Surgeon clearance.
Complex Reconstruction Track (Tendon Transfer, Extensive Tendinosis, Grafting, and/or Corrective Ost
Applies to: peroneal tendon reconstruction with graft, tenodesis/transfer, or combined realignment osteotomy where you prefer casting until 6 weeks.Phase 0: Protection (0 to 6 weeks)Immobilization / WB
- Splint initially, then short-leg cast (your preference: cast through 6 weeks).
- NWB for 6 weeks (unless your osteotomy/fixation construct and soft-tissue quality support earlier progression—your call).
ROM
- Typically no ankle inversion/eversion during this period.
- If you allow any motion: limit to gentle DF/PF only, low amplitude.
Key precaution supported by graft-reconstruction literature
- Avoid inversion-eversion early to prevent stretching/elongation of the healing reconstruction and loss of strength. (PMC)
Phase 1: Transition to Boot + Protected Motion (6 to 10 weeks)
- Convert cast → boot.
- Start progressive WB in boot (often partial → full).
- Begin DF/PF AROM/PROM; introduce inversion/eversion gradually only when you feel the construct is ready.
Phase 2: Strengthening (10 to 16+ weeks)
- Initiate peroneal strengthening later than the standard track.
- Proprioception and gait retraining.
- Sport progression often shifts later depending on osteotomy healing and tendon quality.
Evidence note: Reviews describing tenodesis/complex repairs frequently use longer casting/immobilization windows (6+ weeks) before transitioning to boot and delaying formal PT. (PMC)
Red Flags / When to Slow Down
- Increasing lateral ankle pain that persists >24–48 hours after therapy sessions
- Reactive swelling, warmth, or wound drainage
- “Popping” sensation or recurrent subluxation feeling
- Calf pain/swelling (rule out DVT urgently)
PubMed (Key Evidence Sources)
- Systematic review of post-op rehab after operative peroneal tendon tears/ruptures (summarizes common immobilization + timing patterns). (PubMed)
- Operative treatment review with a more conservative tenodesis pathway (splint then prolonged casting in some tenodesis cases). (PMC)
- Peroneus brevis reconstruction with tendon graft: 2 weeks NWB cast → boot WBAT; PT focuses DF/PF; inversion/eversion prohibited early (supports your “no aggressive eversion early,” especially for graft cases). (PMC)
This website uses cookies.
We use cookies to analyze website traffic and optimize your website experience. By accepting our use of cookies, your data will be aggregated with all other user data.